Degenerative disc disease (DDD) describes a group of symptoms that results from age-related wear-and-tear of the spinal discs. It could also be a result of an acute spinal injury that causes the spinal column to deteriorate or break down.
Despite its name, degenerative disc disease is, in fact, not a disease. This is a natural occurrence that is a result of aging. The rubber-like discs between the vertebrae that act as shock absorbers allow for bending and flexing of the back. Over time, they become worn out and are unable to provide the highest level of protection. MRIs show some kind of deterioration of the spine in the majority of patients over the age of 60.
Symptoms of Degenerative Disc Disease
Symptoms are dependent on which disc is degenerated. The most common early sign is pain and weakness in the back that oftentimes radiates to another area. The pain can be weak to the point where it is almost nonexistent or very severe and prevents a person from continuing daily activities. Even if a person typically only has weak or dull pain, they may experience flare-ups of extremely intense pain.
Pain may worsen throughout the day, due to bending, sitting, standing, and walking. Changing positions and continuing to move carefully can help prevent the pain from getting more intense.
The pain begins with damage in the spine, but over time, the discomfort can result in other conditions such as osteoarthritis. Because the pain radiates to other areas of the body, people tend to feel pain and discomfort in their buttocks and upper thigh, as well as tingling in the legs or feet.
When the degenerated disc is in the cervical spine, the neck area, the pain can radiate to the shoulder, arm, or hand.
Another symptom that is possible is for people to experience spinal instability, leading to muscle spasms in the lower back as the body tries to correct and stabilize the vertebrae. These spasms can be very painful.
Treatment Options for DDD
Treatment for degenerative disc disease generally begins with nonsurgical methods. Your doctor will determine the severity of the condition and recommend treatment methods based on your individual pain.
Nonsurgical Treatments Options
-
- Medications: Your physician may suggest taking NSAIDs or over-the-counter pain relievers such as aspirin or ibuprofen. These help inflammation that can ease your pain and lessen swelling.
- Physical Therapy: A physical therapist can help teach proper exercises to strengthen and stretch the correct muscles that help the back heal. Learning movement modifications to everyday tasks can help prevent painful flare-ups. Specific movements make the muscles in the neck and back stronger and more flexible, allowing better spinal support.
- Epidural Steroid Injections: These injections are minimally-invasive and help reduce inflammation and nerve compression from the collapsing disc space. The injection contains a corticosteroid and an anesthetic numbing agent.
For most patients, physical therapy, in conjunction with pain medication, is enough long-term pain relief.
Surgical Treatment Options
If non-invasive treatment options do not work or if a person continues to experience severe pain, your physician may recommend surgery.
Surgery may include the removal of the degenerated disc, which is then replaced with a new disc. Another option is a partial disc removal (discectomy) to help relieve pressure from your nerves.
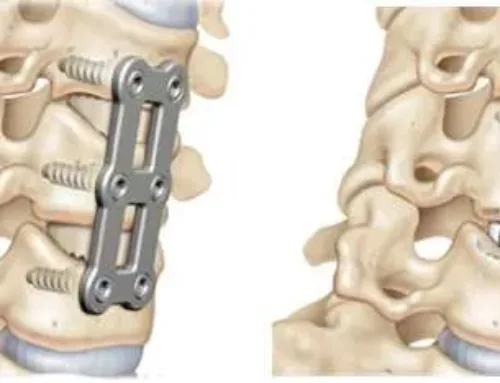
If there is a severe issue, your doctor may permanently connect (fuse) the bones in your spine after the disc is removed. This will reduce the movement in the damaged area.
Along with following your doctor’s treatment recommendations, self-care goes a long way in reducing pain and strengthening your spine. Physical activity and healthy lifestyle choices like a balanced diet, reducing mental and emotional stress, and stopping smoking have profound effects on this type of musculoskeletal condition.
Contact First State Spine for a consultation and to learn what treatments are best for you.
Sources:
Hopkins Medicine: Degenerative Disc Disease
Medical News Today: All About Degenerative Disc Disease
Arthritis.Org: Degenerative Disc Disease